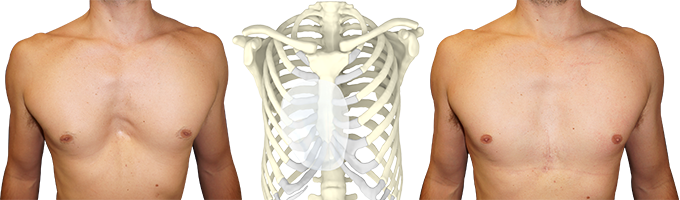
Case presentation
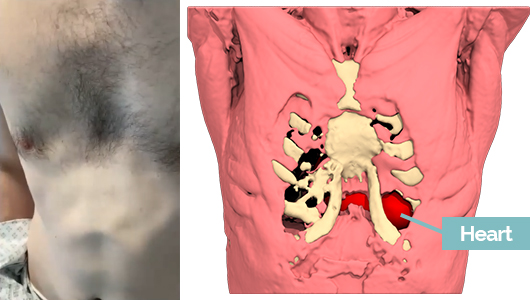
A 38-year-old male presented with a significant pectus deformity with visible apex beat, with no impact on day-to-day activities. Relevant background history included a previous Ravitch Procedure. A computed tomography (CT) thorax demonstrated a Haller Index of 3.5:1. It was used to create a custom-made 3D silicone implant.
Surgery
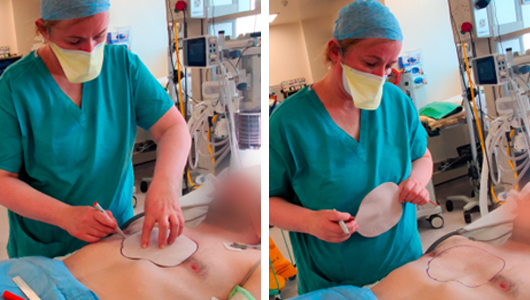
The patient is positioned supine, chest is shaved and IV antibiotics are given intraoperatively. The implant technique is straightforward, there are marks on the implant indicating the proximal and distal marks measurements from the suprasternal notch on the implant and where the midline is. Drawing the outline of the implant with the indicates how much tissue needs to be mobilised to seat the implant.
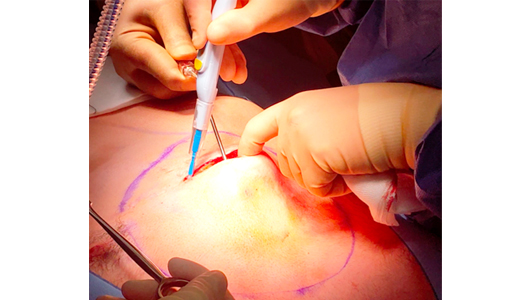
The previous scar was used (instead of the usual midline scar) for improved cosmesis. Ligasure and argon are used as haemostatic devices to keep the wounds dry and limit seroma formation.
Due to the patient's previous surgery there was a large pocket already formed anterior to the sternum. We notice a fracture and defect in the chest wall from Ravitch procedure. A Four-layer polyproline mesh was sutured to cover the chest wall defect providing support for the chest wall and allowing for stabilization of the implant to this mesh.
A four centimeter cut was made on the lower pole of the implant to be inserted, so it can straddle the intra-muscular septum created by the superior aspects of the recti muscle insertions. The implant will be invisible under the fascia and epigastric skin.
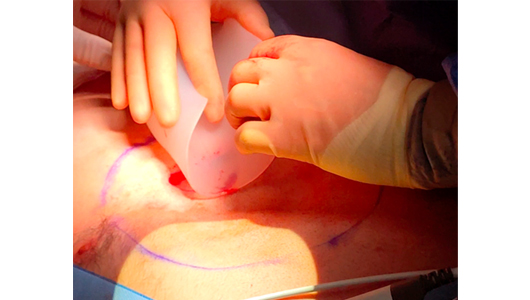
Operation follow-up
A negative pressure wound therapy device is worn for 2 days post-operation to limit the formation of a seroma. This seroma is removed using aseptic technique the day after surgery, and in post operative clinic if required. The patient wore a compressive vest for six weeks post-operation. Contact sports are contra-indicated for 3 months.
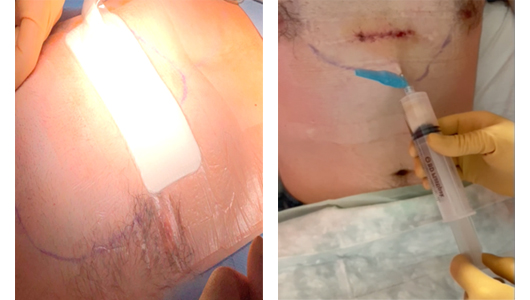
Outcome
The patient achieved his desired cosmetic outcome.
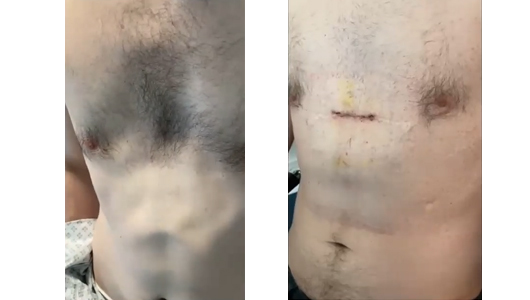
Author and bibliography
Author
Professor Karen Redmond is a thoracic surgeon specialized in lung cancer as well as diseases related to airways and chest deformities.
She graduated from Dublin College in 1997 with honors, receiving the gold medal in surgery. Then she developed her skills in "minimally invasive" surgical techniques for lung cancer as well as in thoracic surgery at Toronto General Hospital (Canada).
She is one of the first surgeons to be trained in robotic surgical techniques and has published comparative meta-analyzes on robotic lobectomy and thymectomy.
Very focused on medical innovation, she does not hesitate to discover and experiment with new surgical techniques to provide the best response to the pathologies of her patients and does not hesitate to treat complex cases of Poland Syndrome and Pectus Excavatum.